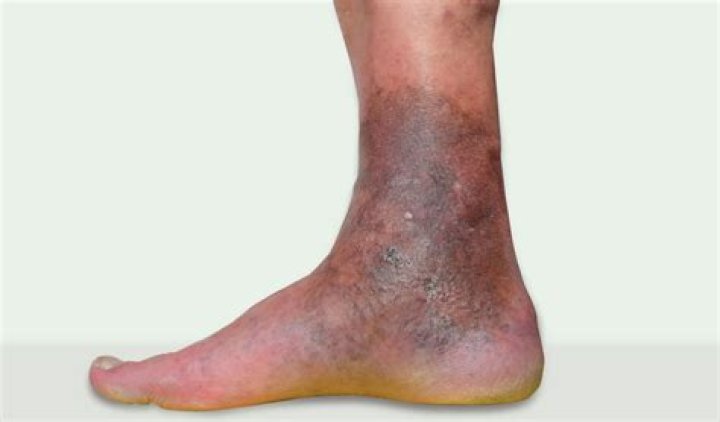
How is Lipodermatosclerosis treated
 Robert Guerrero
Robert Guerrero Lipodermatosclerosis is best treated with conservative management. This includes leg elevation, compression stockings, lifestyle modifications (increased physical activity and weight loss, smoking cessation). Physical therapy using ultrasound has been reported as helpful.
How do you get rid of lipodermatosclerosis?
Lipodermatosclerosis is primarily treated with compression therapy to improve venous insufficiency. Other strategies for managing venous insufficiency include leg elevation; not sitting or standing in one place for long periods of time; regular exercise; and weight loss if overweight or obese.
Is lipodermatosclerosis painful?
Lipodermatosclerosis (LDS) is considered a type of panniculitis (inflammation of subcutaneous fat). Patient experiences severe pain, increased stress, swelling, walking problems and decreased quality of life.
Is lipodermatosclerosis serious?
In addition to poor cosmesis, CVI can lead to chronic life-threatening infections of the lower extremities. Pain, especially after ambulation, is a hallmark of the disease. CVI causes characteristic changes, called lipodermatosclerosis, to the skin of the lower extremities, which lead to eventual skin ulceration.Is lipodermatosclerosis common?
Lipodermatosclerosis is common, affecting middle-aged or older people. It is more common in women and is associated with immobility and a high body mass index (obesity) [1].
Is sclerotherapy considered surgery?
Sclerotherapy involves a doctor injecting a solution into blood vessels or lymph vessels that causes them to shrink. It can help with varicose veins or spider veins. Sclerotherapy is a nonsurgical procedure.
Can you cure Lipodermatosclerosis?
Lipodermatosclerosis is best treated with conservative management. This includes leg elevation, compression stockings, lifestyle modifications (increased physical activity and weight loss, smoking cessation). Physical therapy using ultrasound has been reported as helpful.
What is a Lipodermatosclerosis?
Lipodermatosclerosis (which may be acute or chronic) results from chronic inflammation and fibrosis of the dermis and subcutaneous tissue of the lower legs. Acute lipodermatosclerosis (sclerosing panniculitis) is characterized by painful inflammation above the ankles, which may be mistaken for cellulitis or phlebitis.What happens if chronic venous insufficiency is not treated?
Untreated venous insufficiency results not only in a gradual loss of cosmesis but also in variety of complications including persistent pain and discomfort, hemorrhage, superficial thrombophlebitis, and progressive skin changes that may ultimately lead to ulceration.
How do you improve venous insufficiency?- Keep your legs elevated whenever possible.
- Wear compression stockings to apply pressure to your lower legs.
- Keep your legs uncrossed when seated.
- Exercise regularly.
What foods help venous insufficiency?
- Avocado: contains important minerals that can help prevent varicose veins. …
- Leafy greens.
- Broccoli.
- Brown rice.
- Air-popped popcorn.
- Oatmeal.
- Lentils.
- Barley.
What is the purpose of compression therapy?
Compression therapy is thought to improve performance, reduce soreness after exercise, and reduce the risk of blood clots. Research studies show mixed results. One of the difficulties in measuring benefits is that athletes use many types of stockings and other garments with different levels of compression.
What is Panniculitis?
Panniculitis an umbrella term that describes inflammation in the bottom layers of the skin. It can be caused by a variety of infections, diseases, or external stimuli. Because it can have so many causes, it can be difficult to diagnose.
Why are the bottom of my legs sore to touch?
Pain or tenderness in legs is not a normal condition. One of the most common causes of pain in the lower extremity is venous insufficiency, a condition in which the veins stretch over time and the one-way valves in the veins fail. This valve failure allows venous blood to flow down the leg due to the effect of gravity.
Does venous insufficiency ever go away?
The problem will not go away if you wait, and the earlier it is diagnosed and treated, the better your chances of preventing serious complications. Symptoms include: Swelling in the lower legs and ankles, especially after extended periods of standing.
Is venous insufficiency life threatening?
Venous insufficiency is a common condition. It is not life-threatening, but it is usually chronic. Symptoms of venous insufficiency include varicose veins, swelling, and heavy, aching legs.
Does weight loss help venous insufficiency?
Weight loss does not resolve venous insufficiency, or leaky veins, but treating those veins can relieve leg pain, fatigue, and swelling, which in turn can help patients lose weight.
What are the dangers of sclerotherapy?
Sclerotherapy risks, side effects, and complications include hyperpigmentation, temporary swelling, capillary dilation (telangiectatic matting), pain from the injection, localized hives, tape compression blister, tape compression folliculitis, and recurrence, vasovagal reflex, localized hair growth (hirsutism), skin …
What happens if you don't wear compression stockings after sclerotherapy?
Therefore, it is our practice at EMA to order compression stockings after sclerotherapy treatment. If you choose NOT to wear the compression, you acknowledge that you are at higher risk for complications, in particular: HYPERPIGMENTATION: This is a brownish discoloration which can appear several weeks after treatment.
Which is better for spider veins laser or sclerotherapy?
Sclerotherapy is best for superficial spider veins on the legs and hands. It’s less expensive, faster, and more effective than laser treatment. Sclerotherapy is also better for people with darker skin. Lasers produce light that can cause discoloration in people with tanned skin.
Does walking help venous insufficiency?
Exercise is a surprisingly effective treatment for venous insufficiency. Exercising gets your heart pumping, and the extra pumping force of your heart pushes the blood up and out of your lower legs. Walking is particularly beneficial.
What is a sclerotherapy procedure?
It’s often considered the treatment of choice for small varicose veins. Sclerotherapy involves injecting a solution directly into the vein. The sclerotherapy solution causes the vein to scar, forcing blood to reroute through healthier veins. The collapsed vein is reabsorbed into local tissue and eventually fades.
What causes venous insufficiency?
- High blood pressure in the leg veins over time, due to sitting or standing for long periods.
- Lack of exercise.
- Smoking.
- A blood clot in a deep vein, often in the calf or thigh (deep vein thrombosis)
How do you unblock veins in your legs naturally?
- Exercise. …
- Compression stockings. …
- Plant extracts. …
- Dietary changes. …
- Eat more flavonoids. …
- Herbal remedies. …
- Choose non-restrictive clothing. …
- Keep the legs elevated.
Can venous insufficiency lead to amputation?
The risk of amputation primarily comes from two common vascular diseases, peripheral artery disease (PAD) and venous insufficiency. Both conditions are progressive diseases. As they get worse and the disease progresses, you experience different symptoms.
What vitamin is good for your veins?
Vitamin B. This family of vitamins is among the most important to strengthen your blood vessels and thus, prevent vein issues or at least keep them at bay if they’re already surfaced. For those who have a history of vein issues and blood clots in their family, vitamins B6 and B12 are particularly important.
What juice is good for varicose veins?
The enzyme bromelain, found in pineapple juice, helps reduce fibrin in your veins and can also break up blood clots, a rare but serious potential complication of varicose veins.
Are Raisins good for varicose veins?
Fiber: Dietary fiber intake can help to keep veins healthy. Examples of beneficial fiber-containing foods include: whole grains, brown rice, beans (such as lima and kidney beans or lentils), potatoes with skin, broccoli, cabbage, nuts, fruits (like apples, raisins and berries) and more.
When should compression therapy be used?
Compression is the cornerstone of therapy for patients with venous ulcers. This treatment modality is reported to improve the rate of ulcer healing, reduce the incidence of recurrence, and prolong the time to first recurrence. Between 50% and 60% of patients heal with compression therapy alone during a 6-month period.
How often should you do compression therapy?
How Often Should You Do Compression Therapy? While you will feel great after just one session, like all therapies repeated use yields the greatest benefits. Generally speaking, a healthy individual can use compression therapy 4-6 times per week.
How much pressure at the ankle is required for effective therapeutic compression?
A pressure of 30–40 mmHg at the ankle is recommended for ulcer healing.





